What is the difference between the FDA and CMS?

Although the FDA and CMS regulate different aspects of healthcare — the FDA regulates the marketing and use of medical products, while the CMS regulates reimbursement for healthcare products and services. health care for two of the largest health care programs in the country (Medicare and Medicaid) —the two agencies share a critical interest in …
What is the function of CMS? The Centers for Medicare & Medicaid Services (CMS) provides health coverage to more than 100 million people through Medicare, Medicaid, the Child Health Insurance Program, and the Medicare Market. -Health Insurance.
Is FDA under CMS?
The Food and Drug Administration (FDA) and the Centers for Medicare & Medicaid Services (CMS), both part of the Department of Health and Human Services, and hereinafter ‘ also referred to as « Federal Partners, » agree to work together to promote initiatives related to the review and use of FDA-regulated drugs, …
What is the difference between FDA and Medicare Medicaid Services?
The Food and Drug Administration (FDA) is the gateway through which new drugs and medical devices must pass through to reach the U.S. market, while the Centers for Medicare and Drug Services Medicaid (CMS) determines how products will be reimbursed under Medicare, the largest public health service. insurance program.
What services do the FDA provide?
The Food and Drug Administration is responsible for protecting public health by ensuring the safety, efficacy, and security of human and veterinary drugs, biological products, and medical devices; and by ensuring the security of supply of our nation’s food, cosmetics, and radiation emitting products.
What is the functional difference between the FDA and CMS?
These two agencies have distinct (though related) statutory mandates to apply in their decision-making: The FDA approves drugs and devices based on evidence that the product is « safe and effective, » while CMS makes determinations. of coverage based on whether the product is â € œreasonable and necessary.â €
How does FDA and CMS influence nursing practice?
The agency provides nurses with the most up-to-date data on foods and drugs that are safe and treat patients’ health issues in the most effective way (â € œAbout FDA, â € 2018). Therefore, it simplifies the work of nurses as they have a solid base of medicines to choose from for their patients.
How does CMS influence health care organizations?
CMS manages quality programs that address many different areas of healthcare. These programs encourage quality improvement through payment incentives, fee reductions, and health care quality reporting information on government websites.
What is the role of the CMS in regulating health care?
The CMS oversees programs including Medicare, Medicaid, the Child Health Insurance Program (CHIP), and the state and federal health insurance markets. CMS collects and analyzes data, produces research reports, and works to eliminate cases of fraud and abuse in the healthcare system.
What is the basis of the labor related share?
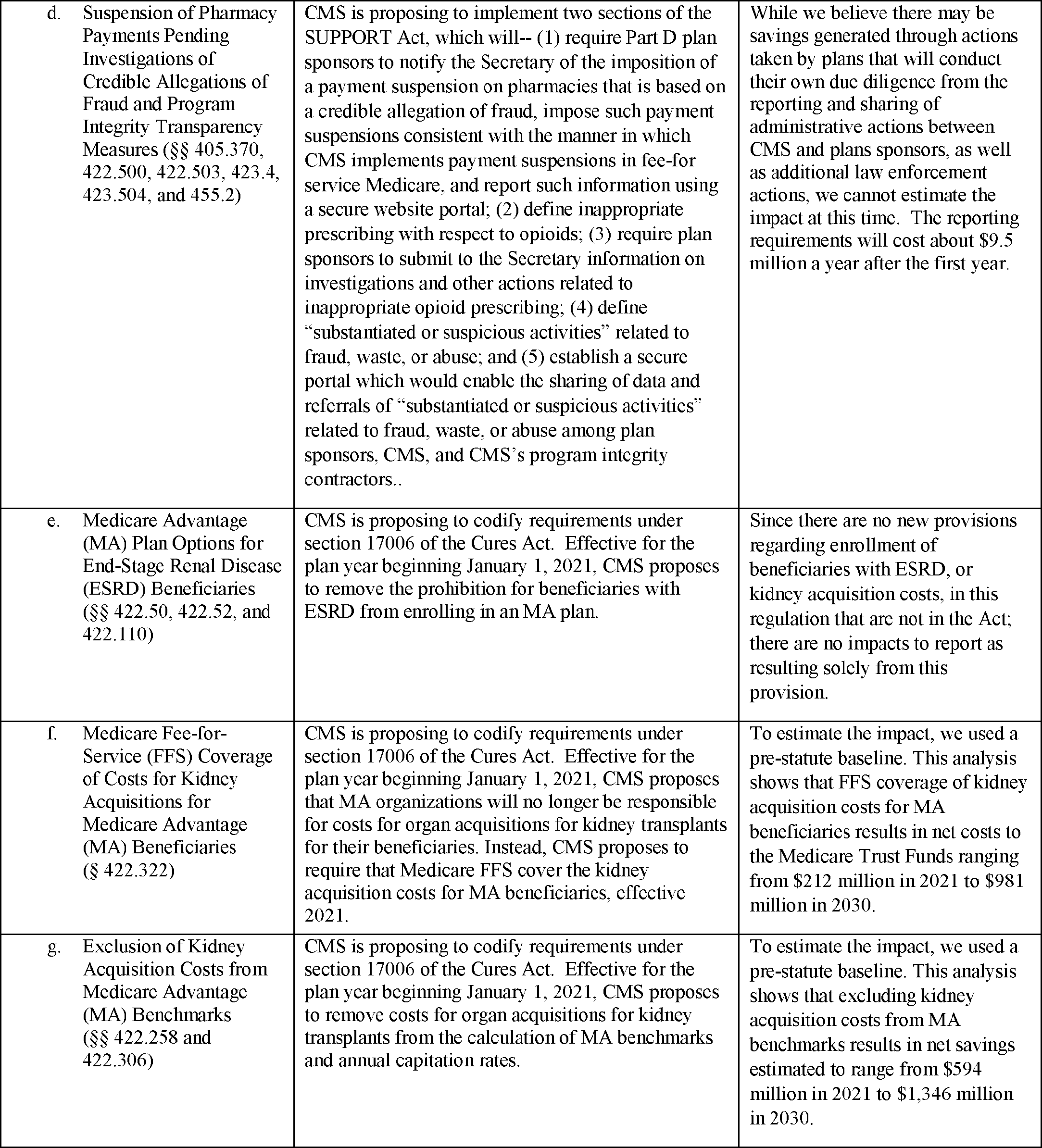
The base payment rate, or standardized amount, includes a labor-related and non-labor-related share. The labor-related share is adjusted by a wage index to reflect area differences in labor cost. If the area wage index is greater than 1.0000, the share of labor is equal to 68.3 percent.
What is the current Medicare base rate? Medicare base payment amounts For fiscal year 2022, the base operating rate is $ 6,122 and the capital rate is $ 473.
What is DRG payment based on?
Diagnosis-related group reimbursement (DRG) is a reimbursement system for inpatient payments from facilities. This system assigns payment levels to each DRG based on the average cost of treatment of all TRICARE beneficiaries in a given DRG.
What type of diagnosis is the MS-DRG prospective payment rate based on?
The MS-DRG is linked to a fixed fee based on the average cost of treating patients in the group. Patients may be assigned to MS-DRG based on their diagnosis, surgical procedures, age, and other information.
How does DRG affect payment for healthcare?
The introduction of DRGs has shifted payment from a cost-plus structure to a flat-rate structure. Under a case-rate reimbursement, the hospital is no longer paid for a patient with a longer stay, or days in higher-intensity units, or receiving more services.
How is DRG payment calculated?
The MS-DRG payment for a Medicare patient is determined by multiplying the relative weight of the MS-DRG by the mixed hospital rate: MS-DRG PAYMENT = RELATIVE WEIGHT × HOSPITAL RATE.
How is the DRG calculated?
The calculation of DRG payments involves a formula representing the adjustments discussed in the previous section. The weight of the DRG is multiplied by a « standardized amount », a figure that represents the average price per case for all Medicare cases during the year.
How are DRGs weighted?
The relative weights of the DRG are estimates of the relative resource intensity of each DRG. These weights are calculated by estimating the average resource intensity per case per DRG, measured in dollars, and dividing each of those values by the average resource intensity per case for each DRG. All DRG, also measured in dollars.
What is the basis of the IPPS?
IPPS pays a flat rate based on the average fees in all hospitals for a specific diagnosis, regardless of whether that particular patient is more or less expensive. Everything from aspirin to artificial hips is included in the price of the package for the hospital.
What is the IPPS?
The Medicare Inpatient Prospective Payment System (IPPS) was introduced by the federal government in October, 1983, as a way to change hospital behavior through financial incentives that encourage more cost-effective management of medical care.
What is covered under IPPS?
acute care of inpatients and agree to accept predetermined rates of the Inpatient Prospective Inpatient Payment System (IPPS) as a full payment. Inpatient hospital benefit covers beneficiaries for 90 days of treatment per episode of illness with an additional 60-day life reserve.
What is the 2021 conversion factor?
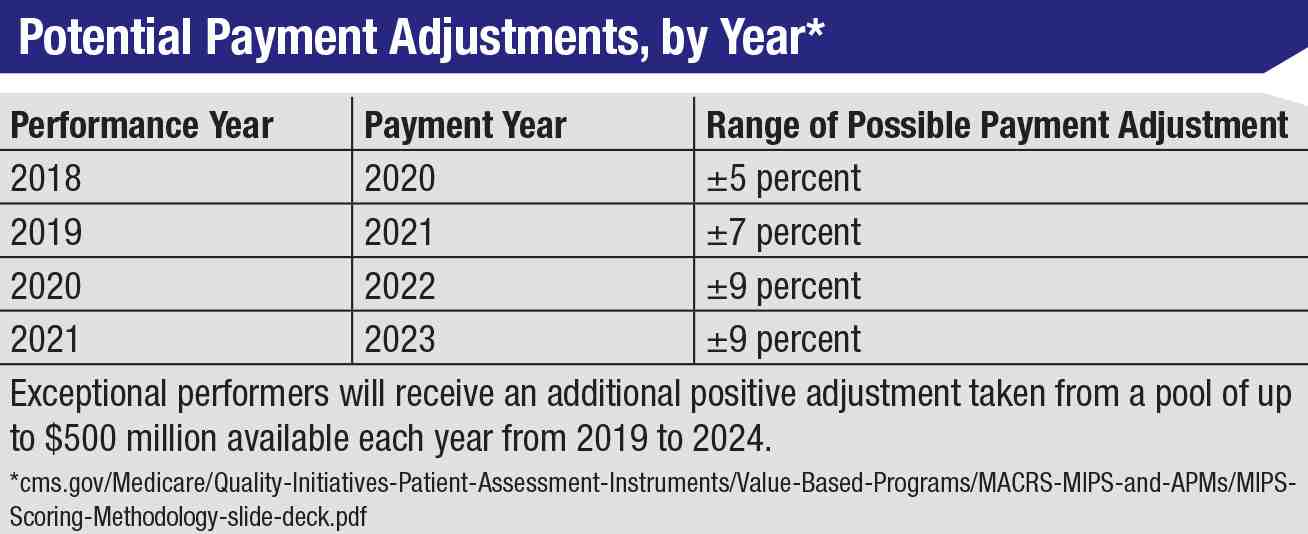
This is slightly less than the 2021 conversion factor of $ 34,8931, but more than the $ 33.59 that CMS planned to implement before S. 610 passed. The new conversion factor is included in updated spreadsheets on the CMS website.
What is the 2021 Medicare Rate? The current tax rate for social security is 6.2% for the employer and 6.2% for the employee, or 12.4% total. The current Medicare rate is 1.45% for employers and 1.45% for employees, or 2.9% of the total.
What is the Medicare conversion factor?
In the implementation of S. 610, the Centers for Medicare & Medicaid Services (CMS) issued a conversion factor for the updated 2022 Medicare physician fee schedule (i.e., the amount Medicare pays per Medicare). unit of relative value) of $ 34.6062.
What is the 2021 RVU conversion factor?
Your specialty income and 2020 wRVU value automatically calculates the 2021 wRVU value based on the estimates provided in Table 106 of the PFS CMS. The tool will also show the estimated combined total RVU impact of the 2021 changes, based on the updated conversion factor of $ 34.8921.
What is the conversion factor for 2020?
Conversion Factor 2020 The estimated PFS 2020 Conversion Factor is 36.09, up from 36.04 in 2019. This reflects the adjustment of budget neutrality and the first year of the 0 percent adjustment adjustment factor under the Medicare Access to Medicare and CHIP Re-authorization Act ( MACRA).
What is the Medicare fee for 2020?
For 2020, Medicare Part B monthly premiums and annual reductions are higher than the 2019 amounts. The standard monthly premium for those enrolled in Medicare Part B will be $ 144.60 by 2020, an increase of $ 9.10 from $ 135.50 in 2019.
How is Medicare conversion factor calculated?
Basically, the relative value of a procedure is multiplied by the number of dollars per Unit of Relative Value (RVU) is the fee paid by Medicare for the procedure (RVUW = doctor’s job, RVUPE = cost of practice, RVUMP = bad practice). Conversion Factor (CF) is the number of dollars assigned to an RVU.
Is CMS and Medicare the same?
Centers for Medicare and Medicaid Services (CMS) are part of the Health and Human Services (HHS) and are not the same as Medicare. Medicare is a government-run government health insurance program, which is administered by the CMS.
Is CMS the same as Medicaid? The federal agency that runs the Medicare, Medicaid, and Children’s Health Insurance Programs, and the federally facilitated Marketplace. For more information, visit cms.gov.
Is CMS both Medicare and Medicaid?
Also known as â € œCMSâ €. The Medicare-Medicaid Coordination Office within the CMS is dedicated to ensuring that all people who are eligible for both Medicare and Medi-Cal have access to seamless and long-term services and supports. high quality.
Who is responsible for CMS?
The Centers for Medicare & Medicaid Services, CMS, are part of the Department of Health and Human Services (HHS).
What CMS stands for in healthcare?
Home – Centers for Medicare & Medicaid Services. CMS.
Is CMS part of Medicare?
The Centers for Medicare & Medicaid Services, CMS, are part of the Department of Health and Human Services (HHS).
What is a CMS program?
A content management system (CMS) is a software application that allows users to create, edit, collaborate, publish, and store digital content. CMSes are typically used for enterprise content management (ECM) and web content management (WCM).
What is the final rule CMS?
The final rule adds Star Ratings (2.5 or less), bankruptcy or bankruptcy files, and exceeding an indicated CMS threshold for compliance actions as a basis for a CMS rejecting a new application or application for an expansion of the -service.
What is an example of a DRG?
The top 10 DRGs in general are: normal newborn, vaginal delivery, heart failure, psychosis, cesarean section, newborn with significant problems, angina pectoris, specific cerebrovascular disorders, pneumonia, and -hips / knees. They include nearly 30 percent of all hospital discharges.
What are DRGs in healthcare? A diagnosis-related group (DRG) is a complex case mix system implemented to categorize patients with similar clinical diagnoses in order to better control hospital costs and determine payer reimbursement rates.
What are the DRG codes?
DRG (Diagnosis-Related Group) Codes A diagnosis-related group (DRG) is a system that classifies hospital cases according to certain groups, also called DRGs, which are expected to have a similar use of hospital resources (costs). They have been used in the United States since 1983.
What are DRG types?
There are currently three main versions of DRG in use: Basic DRGs, All Patient DRGs, and All Patient Refined DRGs. Basic DRGs are used by the Medicare and Medicaid Service Centers (CMS) for hospital payments for Medicare beneficiaries.
How do I find my DRG code?
You have a few options when it comes to identifying code. You can search the ICD-10-CM / PCS codebook, contact the coding department and ask for help, or search using a search engine or app on your smart device.
What is an example of MS-DRG?
definition of MS-DRG. For example, a secondary diagnosis of acute leukemia with chemotherapy is used to define MS-DRG 839. Only a secondary diagnosis. Indicates that in order to be assigned to the specified MS-DRG no secondary diagnoses other than those in the specified list may appear in the patient record.
What is another word for diagnostic?
On this page you will discover 19 synonyms, antonyms, idiomatic expressions, and related words for diagnosis, such as: testing, diagnosis, surgical,, prediction, clinical, ultrasound, DNA based, close to patient, imaging and pharmacogenetics.
What is the general meaning of diagnostic?
identification of a particular disease through a combination of signs and symptoms: diagnostic test.
What are DRG types?
There are currently three main versions of DRG in use: Basic DRGs, All Patient DRGs, and All Patient Refined DRGs. Basic DRGs are used by the Medicare and Medicaid Service Centers (CMS) for hospital payments for Medicare beneficiaries.
How are DRG grouped?
DRGs are grouped into Medicare Severity Diagnosis Related Groups and have 25 groups. These include PRE-MDCs, Unrelated Operating Room Procedures, and Invalid and Ungrouped DRGs.
What is MS-DRG and APR DRG?
As with MS-DRGs, an APR-DRG fee is calculated using an assigned numeric weight that is multiplied by a specific dollar-fixed amount per provider. Each APR-DRG basis, however, considers the severity of the disease and the risk of mortality rather than being based on a single complication or comorbidity.

Commentaires récents